Someone on the internet is wrong. Nowhere is this truer than in the realm of natural health. Bloggers with more enthusiasm than critical thinking skills hype the miraculous healing benefits of various natural products.
Coconut oil receives more than its fair share of the natural health hype. But contrary to many other supposedly miraculous natural treatments, there are legitimate, science-based reasons to use coconut oil – and one very good reason not to use it.
Note that this post refers to topical application. Eating coconut oil is delicious, but I doubt it has any effect on acne.
Moisturizes better than dermatologist-favored treatments
Not surprisingly, coconut is great for moisturizing the skin. Or more accurately, it prevents the skin from drying. Skin becomes dry when the water that’s in and between cells evaporates, which happens faster during winter when the moisture difference between your moist skin and dry outside air is larger.
The layer of oil on your skin (sebum) creates a barrier that prevents the water in the skin from evaporating. Applying coconut oil, or any other oil for that matter, also creates such a layer and helps prevent moisture loss.
A 2014 study published in the International Journal of Dermatology tested coconut oil and mineral oil in children with atopic dermatitis (AD), basically a dry and itchy skin.
This image shows the improvements in AD score (SCORAD) and water loss through the skin (TEWL: transepidermal water loss).
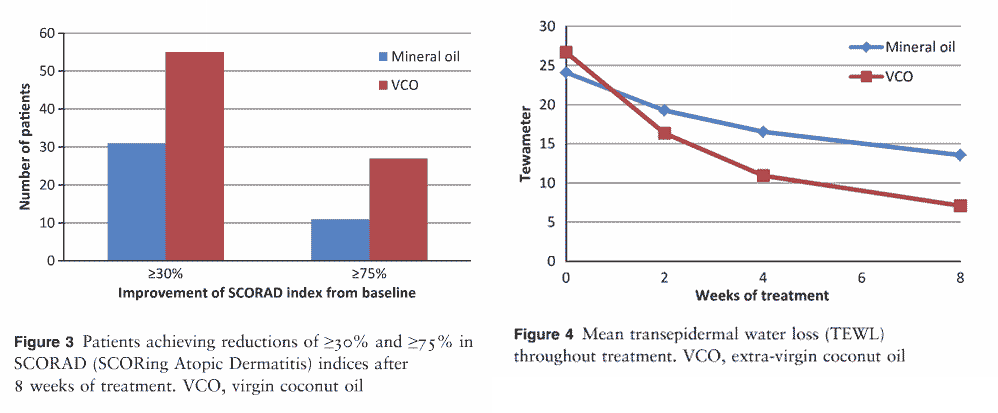
Source: Evangelista, M. T., Abad-Casintahan, F. & Lopez-Villafuerte, L. The effect of topical virgin coconut oil on SCORAD index, transepidermal water loss, and skin capacitance in mild to moderate pediatric atopic dermatitis: a randomized, double-blind, clinical trial. Int. J. Dermatol. 53,100–8 (2014). https://www.ncbi.nlm.nih.gov/pubmed/24320105
As you can see, coconut oil was clearly better than mineral oil in reducing AD score and water loss.
Other studies have come up with similar findings.
TEWL is also important for acne because it indicates how well the skin barrier function works. Poor barrier function leaves the skin vulnerable to infections and colonization by microorganisms.
Stronger anti-bacterial properties than benzoyl peroxide
Coconut oil is strongly antibacterial, which, I believe, is the main reason it could reduce acne.
Lauric acid (LA) is the main fatty acid in coconut oil and accounts for roughly 50% of all the fat. A 2009 study showed LA kills acne causing bacteria 15 times more effectively than benzoyl peroxide.
Another study showed capric acid, another fatty acid in coconut oil, is also effective against P. Acnes bacteria – though weaker than lauric acid.
These studies clearly show that lauric acid is one of the best natural antibiotics against acne-causing bacteria.
However, I should point out that lauric acid in coconut oil is bound to triglycerides – it’s not free. Triglycerides in oils do not penetrate the skin deeper than the first few cells. Oils also have some free fatty acids and the bacteria on the skin can break triglycerides into free fatty acids. So it’s not unreasonable to say oils have some of the effects as their constituent free fatty acids – just nowhere nearly as strong.
Contains anti-inflammatory substances found in high-end skin care products
Coconut oil contains several anti-inflammatory substances, including ferulic acid, p-coumaric acid, and other phenolic compounds. Ferulic acid is used as an antioxidant in many high-end skin care products. There’s some evidence to show these can protect the skin.

One study showed that applying coconut oil to rat ears protected against subsequent chemical exposure. Another study showed that topically applied coconut oil accelerates wound healing.
In the present study, we examined the influence of VCO [virgin coconut oil], applied topically for the healing of dermal wounds in rats. The results indicate a significant beneficial effect of VCO on intracellular and extracellular matrix components and the antioxidant profile during cutaneous wound healing in animals treated.
Nevin, K. G. & Rajamohan, T. Effect of topical application of virgin coconut oil on skin components and antioxidant status during dermal wound healing in young rats. Skin Pharmacol Physiol 23, 290–7 (2010). https://www.ncbi.nlm.nih.gov/pubmed/20523108
But let’s keep in mind that these are animal studies, and nobody can say for sure whether humans using coconut oil at home will get the same benefits.
Still, the anti-inflammatory properties of coconut oil come as a nice bonus, especially given the role inflammation plays in triggering acne.
For best results, use virgin coconut oil. A study showed it has somewhat stronger anti-inflammatory properties than processed coconut oil.
Coconut oil works as a weak sunblock
Coconut oil can also protect the skin against UV radiation. A 2012 study showed that coconut oil blocks around 20% of UVB radiation (and 0% of UVA radiation).
Other studies (here and here (PDF)) have showed that this translates into SPF of around 7.

Just to be clear. Coconut oil is not a sunscreen replacement. It’s not strong enough. But as these studies show, it can protect the damage from occasional UV exposure, which can be helpful for acne-prone skin.
Why?
Many people don’t realize that damage caused by UV radiation (among other things) to sebum is the trigger that kicks off the acne formation process.
Following UV exposure, squalene undergoes massive photodegradation. Upon oxidative challenge, squalene is readily oxidized giving rise to different squalene peroxidation by-products exerting harmful activities in skin..
Squalene peroxide has been demonstrated to be comedogenic: in animal experiments, comedones have been triggered by exposing rabbit ears to irradiated squalene. A positive correlation was found between degree of squalene peroxidation and size of the comedones elicited.
Picardo, M., Ottaviani, M., Camera, E. & Mastrofrancesco, A. Sebaceous gland lipids. Dermatoendocrinol 1, 68–71 (2009). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2835893/
Which is one of the reasons I recommend everyone with acne to use topical antioxidants. Protecting sebum against oxidative damage is one of the keys to preventing acne.
Coconut oil is comedogenic and may cause acne
As promising as these results sound, there’s a caveat. In some cases, coconut oil may also cause acne.
It’s highly comedogenic, rated at 4 at the comedogenicity scale (5 being the maximum rating).
Normally I don’t pay much attention to comedogenicity ratings. They don’t accurately predict whether an ingredient causes acne. In 2006, Greek researchers tested 10 products containing moderately comedogenic ingredients against negative (nothing) and positive (a highly comedogenic ingredient) controls. This graph shows the increase in comedones for each test.

Source: Draelos, Z. D. & DiNardo, J. C. A re-evaluation of the comedogenicity concept. J. Am. Acad. Dermatol. 54, 507–12 (2006). https://www.ncbi.nlm.nih.gov/pubmed/16488305
None of the products containing supposedly comedogenic ingredients caused any more comedones than the negative control. The increase in the graphs is due to the skin being covered with patch testing tape.
Why aren’t comedogenicity ratings useful?
The problem with comedogenicity ratings is that the tests used to derive them just don’t reflect real world usage. In comedogenicity tests, the ingredients are used at very high concentrations, whereas they are used in much lower concentrations in skin care products. Dose matters.
Coconut oil delivers a hefty dose of lauric acid
It’s a bit different when we talk about coconut oil. Earlier I mentioned that coconut oil is about 50% lauric acid, so quite a hefty dose.
It still doesn’t mean coconut oil would cause acne for everyone who uses it. That’s clearly not the case. But it wouldn’t surprise me if it would cause acne to a not insignificant percentage of people.
Beyond that coconut oil seems to be very safe and unlikely to cause contact allergies or other negative reactions.
None of the patients in the VCO group developed adverse reactions. This is concurrent with the findings of our literature search, which showed no published reports of contact dermatitis caused by VCO.
Evangelista, M. T., Abad-Casintahan, F. & Lopez-Villafuerte, L. The effect of topical virgin coconut oil on SCORAD index, transepidermal water loss, and skin capacitance in mild to moderate pediatric atopic dermatitis: a randomized, double-blind, clinical trial. Int. J. Dermatol. 53,100–8 (2014). https://www.ncbi.nlm.nih.gov/pubmed/24320105
Conclusion
Coconut oil stands as an exception among many supposedly highly effective natural acne cures. There are valid, science-based reasons to try applying coconut oil on the acne-prone skin.
Being a relatively heavy oil, it forms a barrier that prevents moisture from escaping and protects the skin. It does this better than dermatologists-favored mineral oil.
Coconut oil can kill acne-causing bacteria. Coconut oil also contains antioxidants and has been shown to offer some protection against UV radiation (but it’s not a substitute for sunscreen!).
On the flip side, coconut oil is highly comedogenic. Comedogenic ingredients are normally not a problem, but given the high dose of lauric acid, coconut oil may cause acne for some people. So I suggest you start carefully and only apply a little bit on a small area of the face.
Coconut oil is an interesting option for people who like ‘all natural’ skincare options. I still believe that properly formulated skin care products that combine antioxidants (vitamin C, green tea, etc.) with antibacterials (tea tree oil), and perhaps salicylic or azelaic acid will prove to be more effective than coconut oil.




Thanks for this well-researched article, I found it extremely helpful. To your knowledge, is there any evidence that oral consumption of coconut oil can have any favorable effects on acne or skin health? Or are the benefits exclusive to topical application?
Glad to hear you liked the post. Honest answer to this question is that I don’t know. As I mentioned in the article, coconut oil has antibacterial properties. As such, it’s not completely implausible that eating coconut oil would kill bacterial overgrowth in the small intestine, a condition that can lead to acne. It’s also possible that those antibacterial fatty acids are transported to the skin where they help to control the acne-causing bacteria. But this is pure speculation from my part and am not aware of any evidence supporting this.
Coconut Oil is extremely comodogenic. But fortunately there’s a solution! Buy Fractionated Coconut Oil. It’s Coconut Oil in liquid form with the lauric acid removed. It’s not comodogenic, so won’t cause your pores and cause you to break out. I wish more people knew about the comodogenic version, because I, too, broke out from unrefined virgin CO.
Removing lauric acid from coconut oil most likely also removes most of its ability to clear acne.
I tried coconut oil over the course of a few months for my chronic adult acne and it just worsened my breakouts and cystic acne. I don’t recommend it, especially if you are prone to cystic acne.
I tried Fractionated Coconut Oil for a couple weeks and I can vouch that I didn’t get any zits over that time. I then combined the FCO with Grapeseed Oil and it kind of came out weird so I stopped using it. But the Coconut Oil without the Lauric Acid was very effective. Now, I will admit that I didn’t have a major issue with zits/acne prior to using FCO but I still would get the occasional zit…yet didn’t get any while moisturizing with Fractionated Coconut Oil.
I would recommend anyone prone to zits to try FCO.
Another great post! Thank you, Seppo!
I personally wouldn’t use coconut oil on my face. But I use olive oil as a cleanser and makeup remover and it hasn’t caused me any troubles. Could you write about olive oil?
One of the best things I’ve done for my skin is using a sunscreen with niacinamide. It’s good in all kinds of weather. So now the only products I use on my face are olive oil, sunscreen, benzoyl peroxide and a moisturizer recommended by Seppo. And my skin looks good.
I can do a post about olive oil, but it won’t happen anytime soon. I need to update my book before putting out more posts. Glad to hear your skin is doing better 🙂
“Coconut oil effectively kills acne-causing bacteria. In fact, it’s 15 times stronger than benzoyl peroxide.”
That can be interpreted wrong. It’s lauric acid that’s 15 times stronger, not coconut oil. You made this clear earlier in the article but I just don’t want people to have the wrong idea at the end.
Yes, you are right. I know that what I said is not technically correct. Free fatty acids can behave differently than fatty acids bound in triglycerides in oil. So it’s somewhat false to claim coconut oil is 15 times stronger than BP, based on a study that showed LA has those properties. Call it journalistic license to simplify things for the sake of social media sharing.
Hi Seppo,
Terrific blog! Really appreciate your balanced views on things.
Regarding the promise of lauric acid against acne: as far as I’m concerned, the studies you refer to have involved *free* lauric acid, whereas in coconut oil the lauric acid is bound up in triglycerides.
Do you have any thoughts on this?
Best regards.
Apologies for late reply. Holiday season at this end of the world.
Yes, you are correct. Recently, I’ve been reading papers regarding what effect fatty acids bound in triglycerides have vs. free fatty acids. The general trend in the papers is that oils have effects that can be, to some degree, predicted by their fatty acid composition. Oils always have some free fatty acids and the bacteria on the skin can break the triglycerides down to free fatty acids. Whether the combination of the two is enough to create an effect on the skin, we can’t say yet.
Anyway, the bottom line is that the post was somewhat erroneous. I edited it to make it clear that studies on antibacterial effects of LA don’t fully apply to coconut oil.
This post is moronic. It says “coconut oil IS highly comedogenic AND that comedogenic products arent normally the problem??
EVERYONE knows comedogenic things cause acne.. thats why its the number one thing acne sufferers look for/ companies always label “non-comedogenic” for that reason..
Nearly everything else on the web says CO is NON comedogenic…
well, honestly their are mixed views, which is bullshit, because it should just be fact that it either is or is not..
But people always say the reason it causes acne at first is simply because your skin is detoxifying itself. It brings things to he surface.. thats why. Im sure the hundreds of people who have said that aren’t just making that up, they’ve seen first hand, their skin was bad and once you wait out the detox period your skin gets better….
This is a common thing when shifting to more natural ways.. switching to natural shampoo’s your hair can have a greasy period at first because its used to producing too much oil because it was stripped of its natural oils. going from a Standard American Diet, to vegetarian or Vegan, you can feel like crap before you get to feel great because your body is making that transition/detoxifying. Hell even just a smoothie cleanse for a week could get people feeling like crap.
Patience is a virtue.
I suggest actually reading the post before condemning it as moronic. In the post, I outlined the reasons why comedogenicity ratings aren’t useful, and I showed studies that prove products with comedogenic ingredients don’t cause acne. Please explain to me how that study is wrong and why we should ignore it.
Everyone ‘knows’ comedogenic ingredients cause acne because this bit of fallacy is uncritically repeated on most beauty blogs. Doesn’t mean it’s true.
Also, anyone who says the skin is ‘detoxing’ doesn’t know what they are talking about. There are no toxins in the skin and nothing to detox. It’s true that the skin may go through an adjustment period when you switch to a different skincare regimen, but this has nothing to do with detoxing.
Seppo,
This product may be the perfect one for those who cannot use the oil,but want to try it for the lauric acid. It’s called Cocolaurin Creme. No oil, just monolaurin and glycerin. Haven’t tried it myself because I’m sensitive to glycerin, but probably most people would tolerate it.
https://www.purehealthforyou.com/monoluarin-faqs/
Do you know if using jojoba oil as a mouisturiser can exacerbate acne? Thanks
I’m not 100% sure, but I think it should be ok. Though, I would recommend rosehip seed, evening primrose, or borage oil as the best oils for acne-prone skin.
Sadly, it caused even my 50+ years mother to brake out (first enlarged pores, later small pimples). To be fair she probably used too much and amount also matters. Still, I never had courage to try it myself after that, I use less comedogenic high lauric acid oil.
I use a tiny amount at night applied with a q-tip and it has reduced my lesions.