Supplement and topical treatment options include vitamin C and B3, diamine oxidase and OTC antihistamine drugs. I recommend taking 1 g of vitamin C per day and using OTC antihistamines as an additional treatment – take one on days you know you can’t avoid histamine-rich foods.
Vitamin C
Vitamin C is critical to the breakdown of histamine. Studies have found a clear correlation between blood levels of vitamin C and histamine – as vitamin C levels drop histamine levels increase.
In a 1980 study, Dr. Clemetson and colleagues analyzed blood levels of histamine and vitamin C from 400 people. This graph shows the relationship between the two:
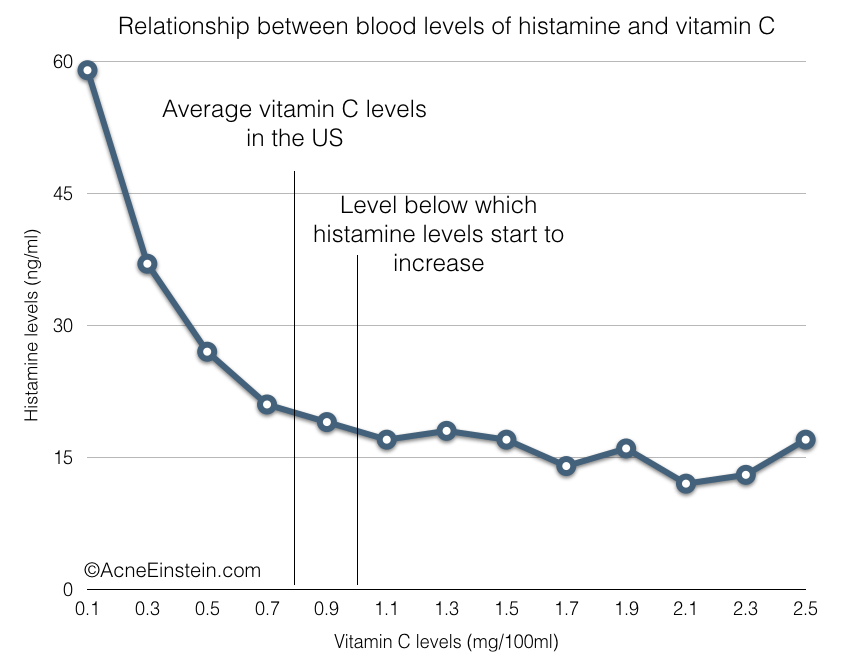
Source: Clemetson, C. A. Histamine and ascorbic acid in human blood. J. Nutr. 110, 662–8 (1980). https://www.ncbi.nlm.nih.gov/pubmed/7365537
Their results showed that histamine levels increased gradually as vitamin C levels dropped below 1mg/100ml. Vit C. levels above 1mg/100ml had no effect on histamine levels.
The blood level of vitamin C at which histamine levels start to increase is fairly high. A 2004 Vitamin C Deficiency and Depletion in the United States: The Third National Health and Nutrition Examination Survey, 1988 to 1994 showed the average vitamin C levels were around 0.8mg/100ml, which is below the 1mg/100ml level at which the histamine levels start to increase.
A 1998 study of vitamin C levels among different ethnic groups in Singapore showed that the average level among all ethnic groups was around 0.6 mg/100ml – well below the 1mg/100ml cutoff point. Likewise, a 1995 study of Slovakian people showed that average vitamin C levels were around 0.5ml/100ml – again, well below the cutoff point.
My point is that you probably don’t consider yourself to be low in vitamin C, it’s not something we usually consider. But these studies show a vast number of people have sufficiently low vitamin C levels that it increases their histamine levels.
Supplementation reduces histamine levels
Dr. Clemetson and colleagues followed up their survey by giving 11 people deemed to have low vitamin C levels and high histamine levels 1 g of vitamin C (as ascorbic acid) for three days. Histamine levels dropped markedly in 10 of the 11 participants.
Other studies have shown similar results:
- Supplementing with 2 g of vitamin C a day reduced histamine levels by 38% in 10 volunteers (source).
- IV injection of vitamin C (7.5 g) reduced histamine levels by 49% in people with allergic disease and by 23% in individuals with infectious disease (source).
- Vitamin C supplementation (up to 250 mg/day) in deficient people reduced histamine levels (source).
Recommendations
Take 1g of vitamin C per day. Just about any vitamin C supplement should do as long as it has ascorbic acid (the most common form of vitamin C).
Diamine oxidase (DAO)
Given that DAO enzyme is the main barrier preventing foodborne histamine from entering the body, supplementing with DAO should also reduce histamine levels.
Unfortunately, I could only find two studies testing this assumption, neither of which was that impressive.
A 2013 study showed a moderate reduction in migraines following DAO supplementation, and a 2016 study showed that 13 out of 14 participants with histamine intolerance noticed a reduction in at least one (of the many tracked) symptoms associated with histamine intolerance.
While DAO supplements are a potential option for histamine intolerance, I wouldn’t recommend them as the main treatment. For several reasons:
- DAO supplements aren’t absorbed and have a short life in the digestive tract, which means you have to take them with every meal with histamine-rich foods.
- DAO supplements are quite expensive. The DAO supplements I saw on Amazon are priced at $1/capsule and more. Given that you have to take them with every meal that contains histamine-rich foods, you could end up paying $120/month for these.
- Anecdotal evidence suggests that DAO supplements alone aren’t very effective.
Bottomline
I would treat DAO supplements as emergency measures. Take them when you can’t avoid high-histamine foods, but don’t rely on them as the primary treatment for histamine intolerance. And they aren’t my first choice as an emergency treatment either. OTC antihistamine drugs are a better option.
Vitamin B6
Vitamin B6 has also been linked to histamine intolerance and treatment recommendations frequently call for B6 supplementation. One of the few studies on this I would find looked at 122 pregnant Hispanic teenagers in Los Angeles. The study showed that teenagers with adequate B6 levels had 38 to 48% higher DAO activity (depending on the measure) than those who were vitamin B6 deficient.
A study comparing eczema and histamine intolerance patients to healthy controls showed no difference in vitamin B6 levels between the groups.
Bottomline
From the data we have, it’s difficult to say whether vitamin B6 supplementation is helpful in histamine intolerance. On the other hand, vitamin B6 supplements are cheap, so there’s little harm in taking one as a ‘just in case’ insurance.
OTC antihistamines
Over the counter (OTC) antihistamines are another treatment option. They are usually sold as allergy drugs.
Keep in mind that antihistamine drugs don’t prevent histamine from being absorbed, they block the effect of histamine by occupying the receptor sites for histamine. The difference can be important. For example, it’s known that high histamine levels depress DAO activity and create this self-sustaining look where high histamine levels reduce DAO activity, which ensures more histamine gets absorbed through the gut. Whether antihistamines can break this loop, I don’t know, but treatments that reduce histamine levels will.
However, antihistamines can have a dramatic effect on acne. Earlier I shared the results of a study that tested antihistamines as an adjuvant (additional) treatment for Accutane. This graph shows the results:
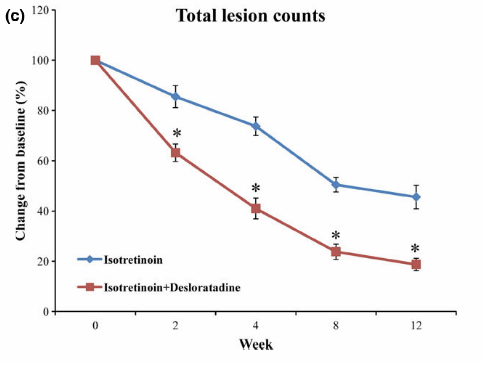
Lee, H. E. et al. Effect of antihistamine as an adjuvant treatment of isotretinoin in acne: a randomized, controlled comparative study. J Eur Acad Dermatol Venereol 28, 1654–60 (2014). https://www.ncbi.nlm.nih.gov/pubmed/25081735
In this study, the researchers used a prescription antihistamine, desloratadine. You can get an OTC version that’s functionally very similar to desloratadine, loratadine. The difference between the two, as far as I can tell, is that desloratadine is a metabolite of loratadine, but they both block the same receptors. Desloratadine is thought to be faster acting and has a longer effect, but, in practice, both should be effective. A pharmacist on Quora claims that pharmaceutically the two drugs are identical.
For all these reasons I recommend loratadine, if you want to try an antihistamine. Brand names include Claritin, Alavert, Reditab, ohm Allergy Relief, and QlearQuil.
You can find countless other antihistamine and anti-allergy drugs on pharmacies. I have no idea whether they are also effective against acne.
Some studies have shown that adding an antihistamine to low histamine diet does not improve the results. With that in mind, I would treat antihistamines like DAO supplements, use to mitigate problems after eating problematic foods. For that purpose, I would recommend antihistamines over DAO supplements. They end up being much cheaper since you have to only take them once a day – as opposed to with every meal for DAO supplements. By all accounts, antihistamines are extremely safe even in long-term use.
Bottomline
I wouldn’t recommend OTC antihistamines as the primary treatment for histamine intolerance. But they can serve as a side-kick. Take one on the days you can’t avoid eating histamine-rich foods.
You can also use them to test whether histamine is a problem for you.
Topical antihistamines
Topical antihistamines and anti-itching creams could also be helpful. I couldn’t find any human studies looking at whether topical antihistamines reduce eczema or other inflammatory skin problems.
Preliminary data shows they can improve skin barrier and reduce inflammation (source, source), and if oral antihistamines reduce acne, then one would think topical antihistamines could also work. But at this point, it’s just not possible to say for sure.
