A UK study from 2012 shows skipping little bit of sleep for a few weeks has no effect on insulin resistance and probably doesn’t hurt your skin. But over time not getting enough sleep is going to get to you and your skin.
Earlier studies have shown sleep deprivation causes blood sugar problems and increases insulin level. In these studies the participants spend anywhere from 1 day to 2 weeks in a sleep laboratory where their sleep is tightly regulated and measured. These studies show fairly drastic results, in some studies insulin levels have increased by 40 to 50% after relatively short sleep deprivation.
Being lab studies, these don’t always reflect real life conditions. People are in an artificial environment where they are constantly prodded and measured. Furthermore, these studies often restrict sleep more than would happen in real life, often allowing participants to sleep only 4 hours.
Short-term sleep deprivation under real life conditions
Last year UK researchers conducted a sleep restriction study that mirrors real life conditions much better. They only restricted sleep 1.5 hours from the participants’ normal sleep duration. So if a person would normally sleep 7.5 hours, they were allowed to sleep only 6 hours. The participants stayed at home and went on with their normal lives.
This study looks like a good indication of what occasionally happens to all of us. Maybe it’s an examination period or you hit a busy spell at work and just don’t have so much time to sleep.
In this study the group of sleep restricted men was compared to another group of similar men who were allowed to sleep normally, giving us a nice comparison.
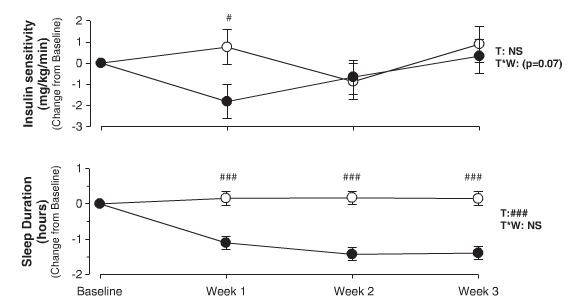
This graph shows insulin sensitivity (opposite of insulin resistance; higher insulin sensitivity means less insulin resistance and less insulin required to clear glucose from bloodstream, and thus also less acne) measures for both groups. The dark circles represent the sleep deprived participants and the white circles the participants who were allowed to sleep normally.
During the first week of sleep deprivation insulin sensitivity dropped quite significantly but recovered during the subsequent two weeks. By weeks 2 and 3 there was no difference between the two groups.
This study suggests that changing how much you sleep causes temporary insulin resistance, but once your body has had time to adapt to the new situation insulin sensitivity is restored. This is also in line with earlier lab studies. Had those studies been continued for longer than a week or two, they might have showed the same recovery.
But wait.. there’s more!
Lack of sleep and junk food
The study also tracked leptin and body weight. Leptin is one of the hormones that control appetite and satiation. Studies have shown that higher leptin levels reduce appetite and the amount of calories you need to eat until you feel satiated.
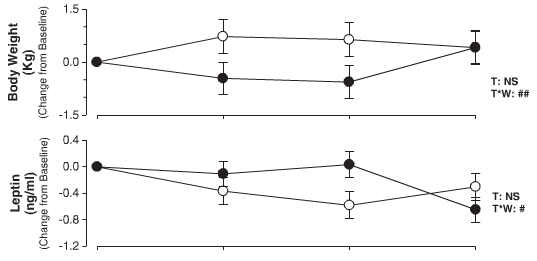
Here are leptin levels and body weight measures for both groups.
Leptin levels took a significant plunge after 3 weeks of sleep deprivation. There was also an increase in body weight at week 3, but it’s hard to say how much of it is due to sleep deprivation and how much just normal variation.
Drop in leptin level could make it harder to stick to healthy diet. Studies show not getting enough sleep makes people more likely to snack and leads to unhealthier food choices (more carbohydrates, more salty snacks). I don’t know about you, but any time I’m really tired, I just can’t be bothered to eat healthy and just gobble down whatever junk happens to lie on my path.
Take away
The take away from this study is that relatively short term, modest sleep deprivation is probably not bad for your skin. Just pay special attention to your food choices during that time, and you probably don’t have to worry about it.
What about long term sleep deprivation?
While short-term sleep deprivation is probably not bad for your skin, there’s good evidence to show long-term sleep deprivation is.
One study compared habitual short sleepers (less than 5.5 hours per night) to normal sleepers (7.5 to 8.5 hours per night) and found that short sleepers were significantly more insulin resistant. Short sleepers required 50% more insulin than normal sleepers to clear identical glucose load.
Epidemiological studies also show fairly consistently that sleep deprivation and sleep problems cause blood sugar problems. Epidemiological studies are studies where a large number of people are followed for a long time (years to decades). They are good at finding associations between variables in real life conditions. The downside is that you can’t determine what causes what from these studies.
Anyway, epidemiological studies show that short sleep or sleeping problems (waking up many times during the night or difficulties in falling asleep) increase the risk of developing type-2 diabetes by 50% to 300% (after controlling for BMI and other covariates).
Take away
The careful take away from these studies is that long-term sleep deprivation can cause insulin resistance and mess up your hormones, and thus be bad for your skin.
Conclusion
The overall conclusion is that modest sleep deprivation (1 to 2 hours) over a week or two shouldn’t be too bad for your skin, as long as you pay careful attention to what you eat during that time and don’t give in to junk food cravings that come with lack of sleep.
In contrast, long-term sleep deprivation is very likely to mess up your insulin and hormone levels and make you more prone to getting acne.
Of course this post only dealt with insulin resistance, which is one of the keys to hormonal acne. Sleep deprivation can (and probably will) also affect other factors behind acne, something I hopefully have time to explore in another post.
Now it’s your turn. Have you noticed any connection between sleep, acne or food cravings? Let me know in the comments below.


>Epidemiological studies are studies where a large number of people are followed for a long time (years to decades)
That would be a cohort study, there’s more to epidemiology than cohort studies, but you probably know that already. Nice to know that my exams aren’t causing insulin resistance though!
True enough. That bit was just there to give people who are not familiar with research methodologies some idea of what those studies are. I try to keep these posts readable to as many people as possible, so I try to keep the technical stuff to minimum. Actually, when I write these posts I have to constantly correct myself and rewrite sentences. After spending so much time reading research literature, I notice that the lingo from those papers creeps into my writing. Something that doesn’t really suit the tone of this blog.
I actually feel like eating less when I am sleep deprived. But the problem is that I’ve been sleep deprived for years. I have had problems with insomnia ever since I was a little child. It’s the most difficult thing to deal with – diet, exercise, etc. I can do them all the right way because I am strong willed but what to do when I just can’t fall asleep no matter how tired I am? Meditation helps to a point but I am still to find the best way to get enough sleep. I only get to sleep well after several days of little sleep. Sleep affects everything in my life. When I haven’t slept enough for too log my heart hurts (literally) – I was really scared the first time I felt that but the doctor said that my heart is absolutely healthy. My acne always becomes worse. Actually my looks mainly on how well I have slept. After a night of great sleep I look radiant and pretty, my skin looks so much better and I receive compliments about the way I look. So the sleep – skin connection is nothing new to me, it’s kind of obvious even without studies. The problem is what to do about it.
Sleep also affects my periods – they are less painful when I get enough sleep or even not painful at all. Strange as it may sound and a bit off topic but regular orgasms help me have a clockwork period exactly 28 days with ovulation on the 14th day) and it also helps with cramps. For women periods play a very important part in acne so I wonder if there are any studies about orgasms and hormonal balance and is it different for men and women. There are studies that clearly show how orgasm helps with cramps but what about long term effects on hormones?
Sorry to hear you have such sleep problems, must make life quite difficult. There’s really nothing I can do for you there as I’m not a specialist in sleep.
AS to orgasms having an effect on hormones. I looked at this for guys since some people claim masturbation and/or sex causes acne. For guys orgasm or ejaculation lowers testosterone level, so that should be good for acne. I can’t say anything about women.
Hi Seppo! I find your posts absolutely awesome. Here’s my case…
You say ejaculation only lowers one’s testo levels so it wouldn’t make one’s acne worse. However in my case, whenever I masturbate, my acne gets worse(just the same kind you had in a photo I found on google, pimples next to my mouth and neck acne, those deeper ones that get inflamed, redness.) I’ve tested this theory many times and often my acne eases after a week or usually two weeks of abstention from ejaculation, but never fully.
I lift weights about 5-6 times a week so I’m wondering whether my acne could be a result from too low a level of testosterone. Also I read a lot about testo->DHT after ejaculation but some say it’s baloney. I know my hormones are pretty f’d up.
I eat multivitamin, vitamin D, zma, acetyl l carnitine + b5, drink at least 3l of water a day, eat healthy food(low carb, but good carbs), I’ve cut down on dairy products quite a lot, drink green tea(big brand though), wash my face twice a day with gentle cleanser and massage cold pressed castor oil and cold pressed virgin coconut oil(coconut oil just started), damping excess oils away, and about every three days wash with a benzoyl peroxide cleanser. I wash with quite warm water(and go to sauna few times a week), and at the end I close my pores with cold water. I use the least oily moisturizer they sell on drug stores, and add a bit of b5 powder to the moisturizer(have found this to ease the inflammation). Recently I started to even swipe my face (after cleansing regimen) with a moist green tea bag. I try pick my face as little as possible, only pimples that have already purged after cleansing regimen. I seldom sleep less than 7 hours per night, usually 8-9h. I don’t have stress(only acne). Still, I have acne. I’m starting to think I’m a lost hope…
Terve Heikki!
Sounds weird. Quite a while back I looked at research regarding T levels and ejaculation. The little there was showed T levels increase little bit during abstinence and drop after ejaculation, which makes sense. Here’s a good article on the topic: https://examine.com/faq/does-ejaculation-affect-testosterone-levels.html
Acne is usually a sign of too much T, not too little. While the evidence is anything but rock-solid, there’s reason to believe many men with acne have elevated androgen levels.
Given all this it sounds really weird that masturbation would cause acne. I’m not aware of any mechanism by which it could happen. Of course this doesn’t mean it’s impossible, just that it sounds really weird to me.
After my last “all-nighter” I broke out horribly! It’s good to understand how it may not have been the sleep deprivation but rather the antecedents. I recall that I was working on a project and was HIGHLY stressed those whole 2 days. Also, when I started to feel tired I just guzzled absurd amounts of caffeine. Double no-no. It would seem that it’s not the sleep deprivation but rather what people do while they’re staying awake. Although, overly anxious people such as myself often work off a lot of tension while asleep; I suspect that if the focus is on stress– then there is a great degree of psychological catharsis which sleep can offer those of us who are wound extra tight.
Agree with you. It’s probably those other things that happen when you are tired that are really bad for your skin.